Plastic surgery procedures can restore balance, refine features, and address changes that occur with age, pregnancy, weight shifts, or genetics. Whether you want to rejuvenate your face, reshape your body, or improve the appearance of your breasts, the right procedure can help you feel more confident and aligned with how you want to look.
Dr. Hayley Brown is board-certified by the American Board of Plastic Surgery. She is an active member of the American Society of Plastic Surgeons (ASPS) and the American Society for Aesthetic Plastic Surgery (ASAPS). She performs all procedures at a fully accredited outpatient surgical center, where Dr. Steve Brown, our in-house board-certified anesthesiologist, administers anesthesia.
In addition to the before-and-after photos on our website, more examples of Dr. Brown’s work are available at Desert Hills Plastic Surgery in Henderson and can be viewed during your consultation. All images are handled in full compliance with HIPAA privacy protections.
Facial Plastic Surgery
Facial procedures help bring out your natural features and enhance facial balance. These treatments are designed to help you look like the best version of yourself by refining areas that may change with age or genetics:
- Eyelid Surgery: Reduces droopy eyelids or puffy under-eye bags, creating a more refreshed appearance.
- Brow & Forehead Lift: Smooths forehead lines and raises heavy brows to open the eyes and brighten your expression.
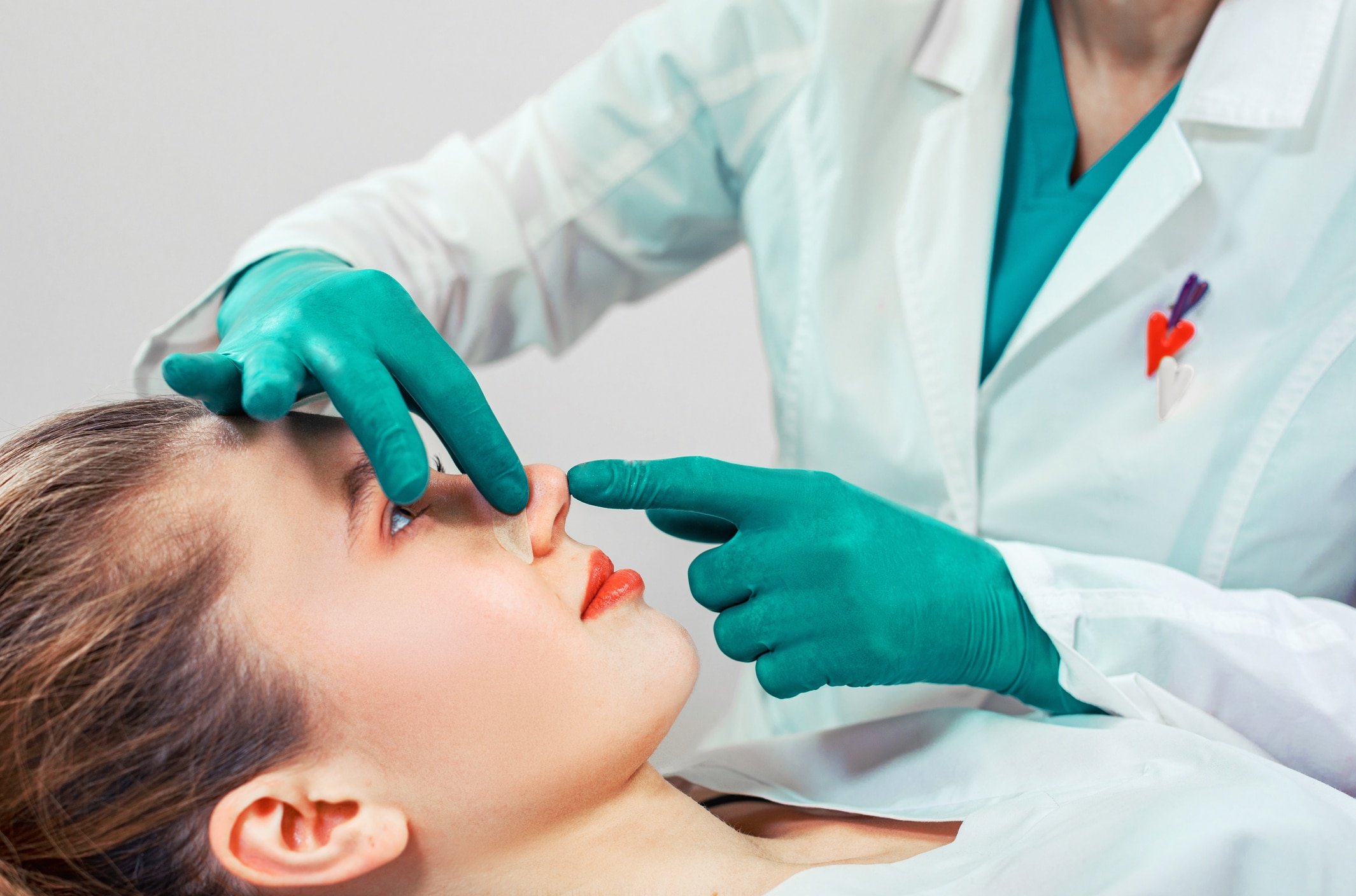
Together, these facial procedures can help rejuvenate your appearance while maintaining your natural look.
Cosmetic Breast Surgery
Breast surgery can change the size, shape, or position of your breasts, depending on your goals. Dr. Brown can create beautiful, custom results with the following surgeries:
- Breast Augmentation: Adds fullness, improves shape, or restores volume with implants.
- Breast Lift: Raises sagging breasts for a more uplifted appearance.
- Breast Lift with Augmentation: Combines implants with a lift, adding fullness and a higher position.
- Breast Reduction: Reduces breast size to create better balance.
- Implant Removal: Removes breast implants for patients who want to go back to their natural size.
- Implant Removal with Lift: Takes out implants and reshapes the breasts at the same time.
- Removal and Replacement of Breast Implants: Remove old or damaged implants and replace them with new ones.
- Nipple Reduction: Reduces the size or projection of the nipples for a more proportionate look.
These breast procedures offer comprehensive options to enhance comfort, restore balance, and help you feel more confident in your appearance.
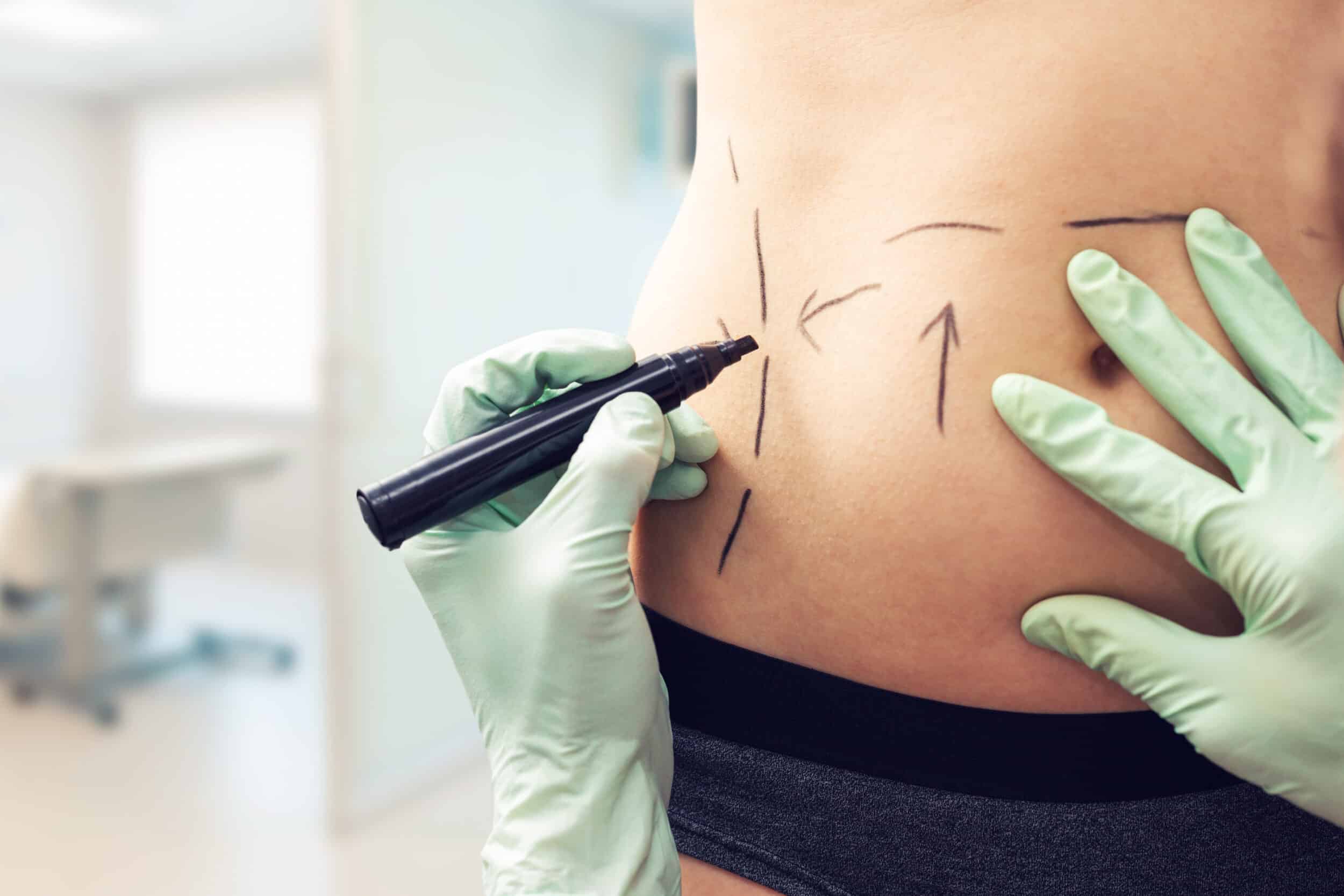
Body Contouring
Body contouring is all about reshaping areas that may not change with diet and exercise. These are your options to smooth out your silhouette:
- Mommy Makeover: A combination of procedures, like a tummy tuck, breast surgery, and liposuction, done together to help restore pre-pregnancy shape.
- Tummy Tuck (Abdominoplasty): Removes excess skin and tightens abdominal muscles.
- Liposuction: Targets stubborn fat in specific areas to create more defined body lines.
These body contouring procedures can refine your shape, enhance symmetry, and help you feel more confident in your appearance.
Non-Surgical Treatments
For patients who want subtle changes without downtime, you can also try our non-surgical treatments. We offer:
- RHA: A modern filler that moves naturally with your expressions.
- BOTOX Cosmetic: Softens wrinkles like frown lines and crow’s feet by relaxing the muscles that cause them.
- Chin Augmentation: Adds definition to the chin with fillers.
- Lip Augmentation: Plumps and shapes the lips.
These non-surgical treatments offer subtle enhancements with minimal downtime, giving you refreshed results while maintaining a natural look.
Why Choose Desert Hills Plastic Surgery?
When you come to Desert Hills Plastic Surgery in Henderson, you are cared for by a team that has been working together since 1996. Your surgery is performed by Dr. Hayley Brown, a board-certified plastic surgeon, while her husband, Dr. Steve Brown, a board-certified anesthesiologist, ensures your safety and comfort. You can feel confident knowing both your surgeon and anesthesiologist are highly experienced.
With Dr. Hayley Brown, you will never feel left in the dark. She will listen to your concerns, explain your options, and give you a clear idea of the results you can expect. Your procedure takes place in a fully accredited surgery center in Henderson, and you will return for follow-up visits so we can carefully monitor your healing and results. Many women choose Dr. Brown because they know they will feel supported throughout the whole process.
Frequently Asked Questions
How Do I Know if I Am a Good Candidate for Surgery?
You may be a good candidate if you are in generally good health, have realistic expectations, and want to improve an area that concerns you. Dr. Brown will review your medical history, discuss your goals, and help determine whether surgery is the right choice for you.
What Should I Expect During My Initial Consultation?
Your consultation is a one-on-one meeting with Dr. Brown where you can talk openly about your goals and concerns. She will review your medical history, examine the area you want to improve, and explain what results you can realistically expect. You will also learn about recovery, potential risks, and alternative options, if applicable.
Before your visit, it helps to research the procedure you are considering, review before-and-after photos, and make a list of questions to ask. Dr. Brown encourages you to take part in the conversation so you leave the decision-making process feeling informed. Phone consultations are available for out-of-town patients.
Are Financing or Payment Plan Options Available?
Yes. At Desert Hills Plastic Surgery Center, we accept cash, cashier’s checks, American Express, Mastercard, and Visa. Financing is also available through CareCredit.
To learn more, you can call CareCredit at 1-800-365-8295 or contact our patient care coordinator for guidance. Please note there is a non-refundable $250 consultation fee, which will be applied to your surgery cost when you schedule.
How Can I Manage Discomfort During Recovery?
Discomfort after surgery is normal but usually manageable. Dr. Brown and her team will provide detailed instructions and, if needed, prescribe medication to help you stay comfortable.
Following your recovery plan, such as resting, wearing supportive garments, and avoiding strenuous activity, will also help promote healing.
What Are the Risks or Complications Associated With Plastic Surgery?
All surgeries carry some risk, but Dr. Brown performs procedures in accredited surgery centers with a board-certified anesthesiologist to maximize your safety. Risks may include bleeding, infection, scarring, or changes in sensation. Dr. Brown will review potential complications specific to your procedure and explain how risks are minimized.
Will Insurance Cover Any Part of the Procedure?
Most cosmetic plastic surgery procedures are considered elective and are not covered by insurance. However, certain reconstructive procedures or medically necessary surgeries may qualify for partial coverage. Our team can help you understand documentation requirements and guide you in verifying your benefits.
What Are the Best Non-Surgical Alternatives to a Facelift?
If you want facial rejuvenation without surgery, options like BOTOX Cosmetic, RHA fillers, and skin resurfacing can soften wrinkles and improve facial contours. These treatments offer natural enhancements but cannot provide the same long-term lifting effects as surgery.
What If I Am Nervous About Undergoing Surgery?
Feeling anxious before surgery is very common. Dr. Brown will take time to explain each step of your procedure, answer your questions, and help you feel prepared. Our team also provides pre-surgical guidance and ongoing support so you feel comfortable throughout your experience.
Will People Know I Have Had Surgery?
Dr. Brown focuses on creating natural results that blend seamlessly with your features. Some swelling or bruising may appear during the early stages of recovery, but this fades with time. Most patients find that friends and family notice they look refreshed rather than surgically altered.
What Is the Most Common Patient Feedback After a Procedure?
Many patients report feeling more confident and aligned with their goals after surgery. They often mention how smooth their experience was with our team and how natural their results appear.
Do Patients Ever Regret Getting Plastic Surgery?
Most patients feel satisfied with their results, especially when they have realistic expectations and choose procedures that align with their goals. Dr. Brown ensures every patient receives honest guidance to support confident decision-making.
How Should I Prepare My Home for Post-Surgery Recovery?
Preparing your home can make recovery easier. Set up a comfortable resting space, gather essentials like pillows, medications, and water, and arrange for help with daily tasks during the first few days. A calm environment supports a smoother recovery.
What Are the Most Common Misconceptions About Plastic Surgery?
Some people believe plastic surgery results always look unnatural, but modern techniques focus on subtle, natural improvements. Others assume procedures are only cosmetic, yet many surgeries also improve comfort and physical function.
What Should I Bring to My Plastic Surgery Consultation?
Bring a list of questions, your medical history, photos of results you like, and any medications or supplements you take. This helps Dr. Brown understand your goals and provide informed recommendations.
Explore Your Plastic Surgery Options in Las Vegas
Find out which Las Vegas plastic surgery procedure is right for you. Please get in touch with Desert Hills Plastic Surgery Center online or call 702-899-1158. Board-certified plastic surgeon Dr. Hayley Brown welcomes patients in Las Vegas, Nevada, and throughout the country.